Ending a round of treatment has typically been a stressful and trying time for cancer patients. With the treatment completed and constant medical supervision ended, the person has had to adjust to everyday life back at home or work. But UHS is changing that.
“Patients are here for two months every day of the week, and when they go home, they can experience the effects of malnutrition and dehydration, just to name two,” explains Jennifer Gusse, RN, BSN, director of Oncology at UHS. “It’s a very critical time, and we want to offer more complete care for these patients.”
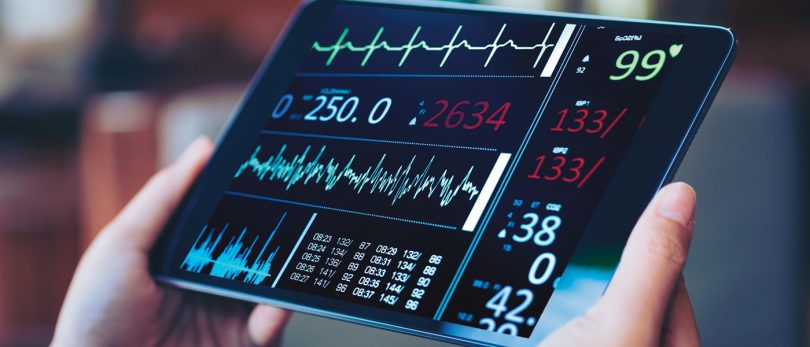
One way UHS is addressing this is through a pilot program for patients with head and neck cancer. At the core of this program is a remote monitoring device that can read patients’ vital signs—such as heart rate, blood pressure or weight, among others—and transmit those readings back to UHS clinicians on a regular basis.
The Care Continuum
Joe Marino, a 57-year-old resident of Endicott, has been using a remote monitoring device as he recovers from four weeks of radiation therapy due to squamous cell carcinoma in his head and neck. “I monitor myself every morning and send in the data every morning,” says Mr. Marino. He explains that when dealing with the challenges of a cancer diagnosis, having someone to check in with every day and look at his vital signs gives him some peace of mind.

After radiation therapy, a remote monitoring device helped Joe Marino stay in touch with his UHS providers on a daily basis.
“I send it in every morning and they let me know that they got my information, and everything is fine,” he says. “They’ll even check on days when I go into the hospital, so on those days I’m basically getting double-checked.”
Rebecca Robins, clinical dietitian and certified specialist in oncology nutrition at UHS Oncology Services, works with Mr. Marino and says that his experience reinforces the reasons UHS implemented this technology in the first place.
“It gives patients reassurance that they are on track and doing what they are supposed to be doing,” says Ms. Robins. “It also helps us show that we still care about their treatment and we’re invested in making sure they have a good outcome.”
Ms. Robins explains that the head and neck cancer patient population was chosen for this pilot program because of the side effects that are often caused by treating these types of cancers: difficulty swallowing and eating and, therefore, difficulty maintaining a healthy weight. Patients like Mr. Marino are often on feeding tubes or limited to easy-to-swallow foods, and this can cause unhealthy weight loss.
With the remote monitoring device, Ms. Robins can determine whether her patients may need follow-up care and reach out to them immediately to ensure it happens. “I have a computer program on my end that receives their data,” says Ms. Robins. “We then compare that to their numbers from previous days and the numbers we take here to see if there is a trend in the data that we need to address with the patient.”
Designing Diets for Cancer Patients
Connecting with Patients
While this remote monitoring program has already proved useful for head and neck cancer patients, the goal is to broaden the use of these devices to not only other cancer services but other UHS services in general. “We’re looking to expand this remote patient monitoring program and use it to create patient plans,” says Michael J. DiFabio, PMP, strategy and performance analyst at UHS.
UHS has recently expanded telehealth services—including offering virtual walk-in care from UHS providers through a web application and in local schools—and will soon integrate Epic’s MyChart into the system, giving patients much more access to their health records and providers. Mr. DiFabio sees remote monitoring as another step in the right direction for UHS to leverage technology to improve the patient experience.
He says some of the areas UHS is considering expanding this program to include patients with chronic obstructive pulmonary disease (COPD) and those with congestive heart failure, among others. Regardless of the type of patient, he echoes Ms. Robins’ and Mr. Marino’s comments in saying it is an important way to continue care, even when patients aren’t regularly in the hospital.
“As healthcare professionals, sometimes we forget that patients don’t know everything we know,” he says. “This program gives them that reassurance that we’re able to check in on them, we can see their results and we can interpret it, so we can bridge that knowledge gap.”
After his experience, Mr. Marino is happy to be a part of a program that will go on to help even more UHS patients. “They should extend [the program],” he says. “I think that is a great idea, especially for people who can’t drive or get there every day.”
Tremendous Tech
The remote monitoring program that helps UHS providers stay in touch with Joe Marino after his treatment is just one of UHS’ ongoing technological initiatives. Whether it is expanding telehealth care to make access to treatment easier for patients across the Southern Tier or bringing virtual walk-in care from UHS providers to your smartphone, computer or tablet, Michael J. DiFabio, PMP, strategy and performance analyst at UHS, explains that careful consideration is taken to ensure these projects are a success for UHS patients and providers.
“We do it the right way,” says Mr. DiFabio. “We do home-grown projects and take the time to make sure they work. For the remote monitoring program [or virtual walk-in], your UHS providers who you see in the office are reviewing your data. The same people you have a bond with and you’ve gone through tough times with are continuing that care even when you’re at home. This makes the experience consistent, and it’s why we stand out from other organizations who might lean on third parties to handle this type of care.”
ANY TIME, ANYWHERE
Start a UHS Virtual Walk-In visit any time at nyuhs.zipnosis.com, and stay tuned to nyuhs.org for updates on our latest technological initiatives.